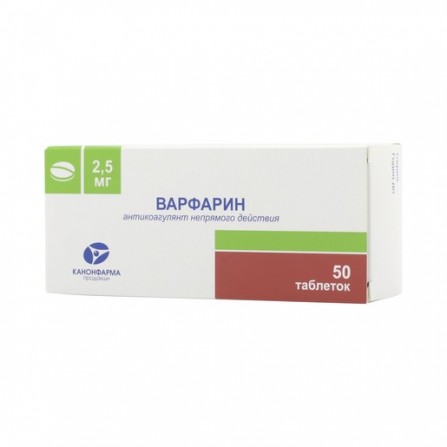
Warfarin Canon pills 2,5mg N50
Condition: New product
1000 Items
Rating:
Be the first to write a review!

More info
Active ingredients
Warfarin
Release form
Pills
Composition
Warfarin sodium 2.5 mg. Adjuvants: calcium hydrophosphate dihydrate - 65.5 mg, microcrystalline cellulose - 60 mg, colloidal silicon dioxide - 1 mg, copovidone - 6 mg, croscarmellose sodium - 4 mg, magnesium stearate - 1 mg.
Pharmacological effect
Indirect anticoagulant. Inhibits in the liver the synthesis of vitamin K-dependent blood coagulation factors (II, VII, IX and X) and proteins C and S in the liver. The optimal anticoagulant effect is observed for 3-5 days from the start of the application and stops 3-5 days after the last dose.
Pharmacokinetics
Absorption and distribution: After oral administration, warfarin is completely absorbed from the gastrointestinal tract. Binding to plasma proteins - 97-99%. Therapeutic plasma concentration is 1-5 mcg / ml (0.003-0.015 mmol / l). It penetrates the placental barrier, but is not secreted with breast milk. Metabolism and excretion: It is a racemic compound, while in the human body, the L-isomer has more activity than the programata. The drug is metabolized in the liver to form inactive and weakly active metabolites that are reabsorbed from bile, while the L-isomer is metabolized faster. T1 / 2 racemic warfarin - 40 hours. Excreted by the kidneys.
Indications
Treatment and prevention of vascular thrombosis and thromboembolism: - acute venous thrombosis and pulmonary thromboembolism arterii- postoperative tromboz- reinfarction miokarda- as additional medicament during surgical or thrombolytic treatment of thrombosis, as well as electrical atrial cardioversion aritmii- recurrent venous re tromboz- pulmonary embolism - prosthetic heart valves and blood vessels (possible combination with acetylsalicylic acid (ASA) - Peripheral, coronary and cerebral artery thrombosis — secondary prevention of thrombosis and thromboembolism after myocardial infarction and atrial fibrillation.
Contraindications
- acute bleeding; - severe liver disease; - severe kidney disease; - renal failure; - severe arterial hypertension; - acute DIC syndrome; - deficiency of proteins C and S; - hemorrhagic diathesis; - thrombocytopenia; - peptic ulcer of the stomach and duodenum in the phase of aggravation; - hemorrhage in the brain; - alcoholism; - pregnancy; - hypersensitivity to the components of the drug.
Dosage and administration
The drug is taken orally, 1 time / day, at the same time.The initial dose is 2.5-5 mg / day. Further dosing regimen set individually depending on the results of determining the prothrombin time or INR. The prothrombin time should be increased by 2-4 times from baseline, and the INR should reach 2.2-4.4, depending on the disease, the risk of thrombosis, the risk of bleeding and the individual characteristics of the patient. When determining the INR, the sensitivity index of thromboplastin should be taken into account and this indicator should be used as a correction factor (1.22 - when using the domestic thromboplastin from the brain of the Neoplast rabbit and 1.2 - when using the thromboplastin made by Rosh Diagnostics). Before the upcoming surgery (with a high risk of thromboembolic complications), treatment begins 2-3 days before surgery. In the case of acute thrombosis, treatment is carried out in combination with heparin until the effect of oral anticoagulant therapy is fully manifested (no earlier than 3-5 days of treatment). When prosthetic heart valves, acute venous thrombosis of the veins or thromboembolism (in the initial stages), left ventricular thrombosis and for the prevention of myocardial ischemia, you should strive for effective action, noted in INR - 2.8-4.0. In the case of atrial fibrillation and during maintenance therapy for venous thrombosis and thromboembolism, a moderate anticoagulant effect is achieved (INR 2-3). When combined with the use of warfarin with ASA indicator INR should be in the range of 2-2.5. Elderly patients and debilitated patients are usually prescribed lower doses. The duration of treatment depends on the condition of the patient. Treatment can be canceled immediately.